J Wave ECG Uncovered: Surprising Insights and Hidden Risks You Need to Know
In the realm of cardiology, the J wave ECG remains a subject of intense research and clinical curiosity. The J wave—a subtle, yet pivotal marker on the electrocardiogram (ECG)—has emerged as an indicator of various life-threatening arrhythmias, including those linked to sudden cardiac death. This phenomenon is not merely an academic curiosity; it holds practical implications that demand our attention. As a burgeoning field of study, understanding the J wave’s nuances can significantly impact patient outcomes and diagnostic precision.
Key Insights
- The J wave ECG, often subtle, signals potential arrhythmias and sudden cardiac death.
- Comprehensive knowledge of J wave characteristics can enhance diagnostic accuracy.
- Implementation of advanced screening and monitoring can mitigate the risks associated with J waves.
Understanding the J Wave
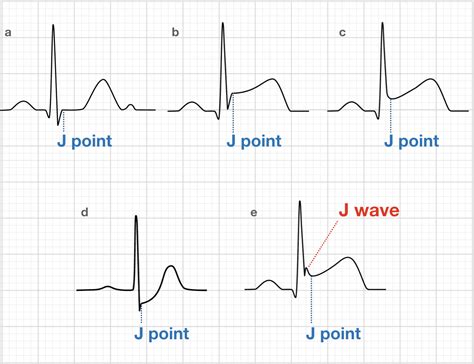
The J wave manifests as a small, abrupt upslope at the junction of the QRS complex and the ST segment on the ECG. Though minimal, this marker is a critical indicator of abnormal electrical activity in the heart. The phenomenon is closely associated with conditions such as Brugada syndrome and early repolarization syndrome. Understanding the precise mechanisms underlying the J wave can significantly bolster the diagnostic framework and enable early interventions.
The importance of recognizing the J wave lies in its diagnostic potential. For instance, in patients presenting with syncope or atypical chest pain, a J wave on the ECG might herald a severe underlying condition that requires immediate attention. Detailed knowledge of the J wave and its correlation with specific clinical manifestations allows clinicians to employ targeted diagnostic tools, such as provocative pharmacological testing, to confirm the presence of underlying arrhythmic conditions.
Clinical Implications and Risk Stratification
The clinical implications of a J wave are profound, particularly in risk stratification for sudden cardiac death. In high-risk populations, the presence of J waves on the ECG necessitates a heightened level of surveillance. These individuals often require comprehensive cardiac evaluations and might benefit from implantable cardioverter-defibrillators (ICDs) to mitigate the risk of fatal arrhythmias.
Advanced screening strategies, such as genetic testing and family history assessments, are paramount in identifying at-risk individuals. In populations where J waves are common, such as those with ethnic predispositions to early repolarization syndrome, widespread screening could drastically reduce mortality rates. The integration of these practices within routine cardiology care represents a crucial step in leveraging the insights provided by the J wave for improved patient outcomes.
What are the primary conditions associated with the J wave?
The primary conditions associated with the J wave include Brugada syndrome and early repolarization syndrome. These conditions often present with life-threatening arrhythmias and can lead to sudden cardiac death if not properly managed.
How can the presence of a J wave be managed clinically?
Managing the presence of a J wave clinically involves comprehensive cardiac evaluations, including provocative testing, genetic assessments, and potential implantation of ICDs. Monitoring and early intervention are key to mitigating risks and improving patient outcomes.
The exploration of J wave ECG unveils a realm where science and clinical practice converge to address some of the most severe cardiac conditions. As we deepen our understanding, the insights gleaned will likely reshape diagnostic paradigms and enhance the precision of risk assessment in cardiology. The J wave, though subtle, carries the potential to save lives, underscoring the importance of meticulous and informed clinical scrutiny.