In the realm of modern medicine, the advancements in minimally invasive ear surgery are transforming patient outcomes and enhancing the quality of care. The emergence of these techniques not only promises reduced recovery times but also aligns with the evolving expectations of patients seeking efficient, effective, and comfortable surgical experiences. This article delves into the intricacies and benefits of these cutting-edge procedures, providing a comprehensive overview for both medical professionals and informed patients.
Key insights box:
Key Insights
- Enhanced patient outcomes: Minimally invasive ear surgeries often result in better hearing and reduced complications.
- Technical considerations: The precision of modern tools and techniques ensures accurate interventions with minimal tissue disruption.
- Actionable recommendation: Patients should consult with ENT specialists to explore the best minimally invasive options tailored to their specific condition.
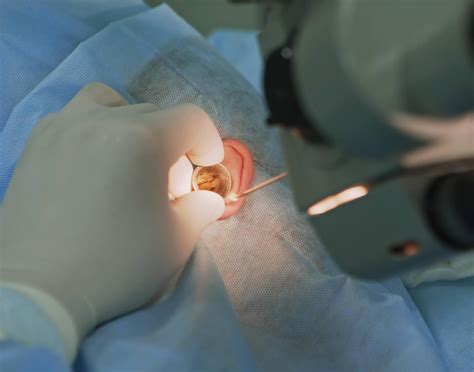
Minimally invasive ear surgery represents a revolutionary approach to treating a variety of ear conditions. This method utilizes smaller incisions and advanced tools, allowing surgeons to operate with higher precision and reducing trauma to surrounding tissues. Traditional ear surgeries often required larger incisions, which led to longer recovery periods and higher risks of postoperative complications. Minimally invasive procedures, on the other hand, leverage endoscopic and microscopic techniques to facilitate surgeries that are less invasive and more precise.
For instance, consider the case of tympanoplasty, a common ear surgery to repair a perforated eardrum. Traditionally, this surgery required a small incision in the ear canal and took weeks for full recovery. With the advent of minimally invasive techniques, surgeons can now perform the procedure through tiny, natural openings in the ear, significantly reducing recovery time and minimizing discomfort. The procedure still achieves the same goals but with less disruption to the patient’s normal life.
Ear surgery advancements are also evident in treatments for chronic ear infections, known as chronic otitis media. Historically, this condition required extensive surgical interventions involving the removal of infected tissue, often resulting in long recovery times and potential hearing loss. With minimally invasive techniques, surgeons can now perform precision interventions that not only target the infection but also preserve as much healthy tissue as possible. This preservation helps in maintaining or even improving the patient’s hearing, resulting in superior long-term outcomes.
While the benefits of minimally invasive ear surgery are substantial, it’s important to understand the context and specific conditions for which these techniques are best suited. Not every ear condition is amenable to a minimally invasive approach, and some cases may still require traditional surgical methods. Therefore, it is crucial for patients to undergo a thorough evaluation by a qualified ENT specialist to determine the most appropriate treatment plan.
FAQ section:
Is minimally invasive ear surgery suitable for everyone?
Minimally invasive ear surgery is not suitable for every patient. The suitability depends on various factors, including the specific ear condition, overall health, and individual anatomy. It is essential for patients to consult with an ENT specialist to determine whether this approach is appropriate for their case.
How long is the recovery period after minimally invasive ear surgery?
Recovery periods for minimally invasive ear surgeries are generally shorter than those for traditional surgeries. Patients can often return to their regular activities within a few days to a couple of weeks, depending on the specific procedure and individual healing rates. However, complete healing may take several weeks, and it’s important to follow post-operative care instructions provided by the surgeon.
In conclusion, the advancements in minimally invasive ear surgery not only enhance surgical precision but also offer significant benefits to patients in terms of reduced recovery times, minimal discomfort, and better overall outcomes. As these techniques continue to evolve, they are set to play a pivotal role in modern otolaryngology, providing hope and improved quality of life for patients with a range of ear conditions.